Diabetes and Gum Disease: Understanding the Link and Protecting Your Oral Health
Diabetes is a condition that affects millions of Australians, having a profound impact on various aspects of their health, including oral wellness. People living with diabetes are at an increased risk of suffering from dental issues such as cavities, gum disease—also known as periodontal disease—and other complications that can exacerbate their diabetes management. In fact, severe tooth loss is notably higher in adults with diabetes, highlighting the importance of oral health in the diabetic community.
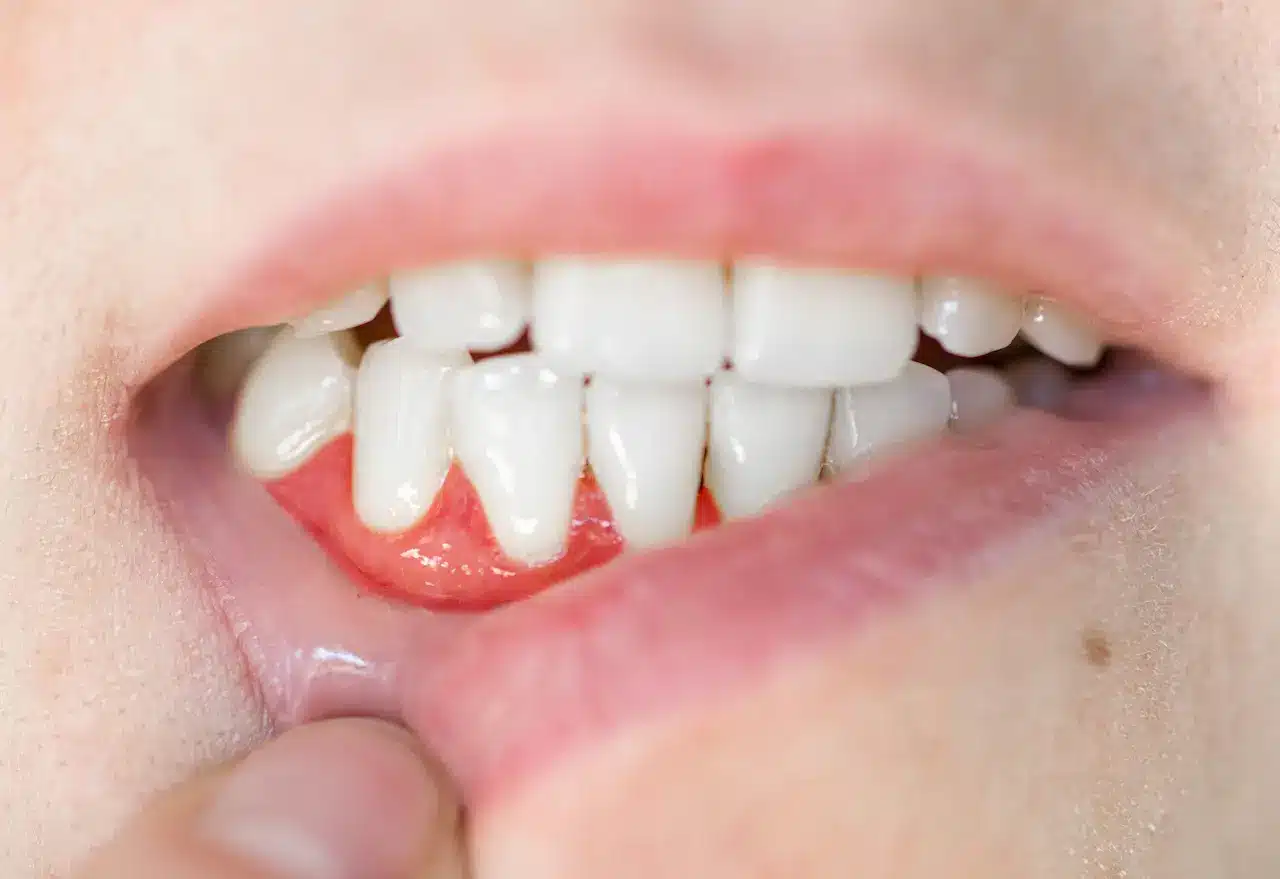
The relationship between diabetes and gum disease is particularly significant, as fluctuations in blood glucose levels can lead to changes in saliva production, creating an environment conducive to oral bacteria growth. This can accelerate the progression of plaque formation, potentially leading to more serious gum infections and tooth loss if not properly managed. Symptoms of diabetes-related gum disease can include tender, bleeding gums or receding gums that can eventually lead to loose teeth.
Management of both diabetes and oral health requires great care. Maintaining blood glucose within the target range, alongside a healthy diet, is crucial. Additionally, regular dental check-ups and cleanings, proper oral hygiene practices at home, and steering clear of smoking can greatly improve oral health outcomes for those living with diabetes. These preventative measures are key to reducing the risk of severe oral health complications and ensuring dental health longevity within the diabetic population.
Table of Contents
Toggle
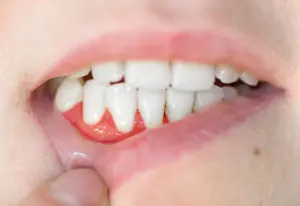
Understanding Gum Disease and Diabetes
Gum disease and diabetes interact in ways that exacerbate both conditions. Effective management is critical to maintain overall health and prevent severe complications.
The Connection Between Diabetes and Gum Health
Diabetes can lead to changes in blood vessels, impairing the supply of nutrients and waste removal, which weakens gums and bones, heightening infection risks. High glucose levels in the blood and saliva promote bacterial growth, increasing the likelihood of gum disease. Gum disease, in turn, may cause blood sugar levels to rise, making diabetes harder to control.
Diabetes-Related Mouth Problems
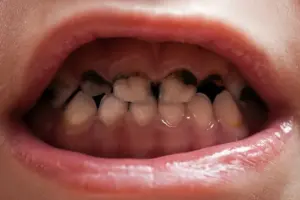
People with diabetes face an increased likelihood of experiencing dental problems due to altered saliva production, leading to drier mouths and higher glucose levels in saliva. This creates the perfect environment for harmful bacteria, which can lead to plaque formation, cavities, and the most severe oral complication, gum disease. Other related issues include thrush, an opportunistic fungal infection, and burning mouth syndrome.
Risk Factors for Gum Disease in Diabetics
Individuals with diabetes who have poor glycemic control are at a higher risk of developing gum disease. Smoking significantly increases this risk. Periodontal diseases range from mild gingivitis to severe periodontitis and can lead to tooth loss. Symptoms to look out for include red, swollen or bleeding gums, and persistent bad breath. Regular dental visits for cleanings and checkups are crucial for early detection and treatment.
Diagnosing and Treating Gum Disease
Effective management of gum disease is crucial, particularly for those with diabetes due to increased susceptibility and the potential for complications around diabetes control.
Diagnosis of Gum Disease
Gum disease is commonly detected during a thorough examination of the mouth, which includes a review of the individual’s health history. Dentists look for signs of inflammation and measure the depth of pockets between the teeth and gums. An important diagnostic tool is the dental X-ray, which can reveal any bone loss around the teeth.

Treatment Modalities for Gum Disease
The treatment for gum disease usually begins with the removal of plaque and tartar beneath the gums, a process known as scaling and root planning. In certain cases, antibiotics may be prescribed to fight off infections. Advanced stages of the disease might require surgical interventions to restore supportive tissues.
Regular dental visits and maintaining high oral hygiene standards are vital in preventing gum disease. Brushing twice daily, flossing, and managing blood glucose levels form the cornerstone of effective prevention. Avoiding tobacco use and eating a healthy diet also contributes significantly to good oral health.
For people with diabetes, it is particularly important to take extra care with oral health to prevent the loop where poor gum health exacerbates diabetes management, and poorly controlled diabetes further impairs gum health.
Prevention of Gum Disease
Preventing gum disease is especially important for people managing diabetes, given their increased susceptibility to such conditions. Proper oral hygiene is fundamental in this preventive approach. This encompasses daily practices such as regular brushing, using fluoride toothpaste, and flossing to remove plaque. Reducing plaque accumulation helps stop the risk of gum infection.
Regular dental check-ups play a vital role in the early detection and management of periodontal diseases. Dentists can provide professional cleanings to remove tartar, which cannot be eliminated by brushing alone. They also offer advice tailored to individual oral health needs.
Controlling blood glucose levels is crucial for overall health and especially oral health for those with diabetes. Elevated levels of blood glucose can contribute to periodontal disease progression. Maintaining a balanced diet, monitoring blood sugar levels, and adhering to diabetes medication can mitigate these risks.
Giving up smoking is key, as smoking significantly intensifies the likelihood of developing gum diseases. The combination of diabetes and smoking can accelerate the severity of periodontal issues.
Additionally, dental professionals may recommend therapeutic mouth rinses and more frequent cleanings to manage gingivitis or mild periodontitis. If the disease has escalated, treatments may include deeper cleaning procedures like scaling and root planing, medications, and in severe cases, surgery.
Key Points for Prevention:
- Practice strict oral hygiene: brush twice daily and floss.
- Schedule regular dental visits for cleanings and check-ups.
- Manage diabetes effectively to keep blood glucose levels in check.
- Quit smoking to decrease the risk of severe gum diseases.
By following these preventive measures, people living with diabetes can significantly reduce the risk of developing serious periodontal diseases, ensuring both dental and general health are maintained.
The Impact of Lifestyle Choices
Lifestyle choices play a pivotal role in the maintenance of oral health, particularly for those with diabetes, as these decisions can directly influence the progression of gum disease and the occurrence of diabetes-related mouth problems.
The Role of Smoking in Gum Disease and Diabetes
Smoking is well-documented as a significant factor in developing gum disease. For people with diabetes, the combination of smoking and high blood glucose levels creates a heightened risk for periodontal disease. This condition frequently starts with inflamed gums and can lead to tooth loss if not addressed promptly. People with diabetes who smoke are also more susceptible to other oral health issues, such as dry mouth, thrush, and tooth decay, due to the constricted blood flow to the gums and altered bacterial presence in the mouth.
Nutrition and Diet Considerations
Diet is another critical aspect of managing both diabetes and gum disease. Consuming healthy meals contributes to keeping blood glucose levels within the target range, which, in turn, lowers the risk of periodontal problems.
- Key dietary advice for oral health includes:
- Eating a variety of nutrient-rich foods to maintain healthy gums.
- Avoiding excessive sugary snacks that can contribute to plaque buildup and cavities.
- Choosing foods that stimulate saliva production to combat mouth dryness.
Proper nutrition also involves adequate hydration, promoting saliva production, which is essential for neutralising the mouth’s pH and reducing bacterial growth. Regular dental checkups are imperative to manage existing mouth problems and advise on dietary choices that support oral health.
Comprehensive Dental Care Strategies
Effective management of oral health for individuals with diabetes is critical due to the higher risk of severe tooth loss and periodontal disease. Consistent dental visits and diligent home care practices help maintain oral health and can positively impact diabetes control.
Regular Dental Visits
Regular dental check-ups are vital as they allow for the early detection and treatment of oral health issues. Dentists can diagnose gum disease through an examination of the gums for inflammation, measurement of pockets around the teeth, and X-rays to detect bone loss. People with diabetes should inform their dentists about their condition, as they need more personalised dental care to manage the relationship between diabetes and oral health.
- Schedule: Adults with diabetes should visit the dentist at least twice a year or as recommended.
- Screening: These appointments include screening for gum disease, cavities, and other common mouth problems like thrush and dry mouth.
- Professional Cleaning: Treatments may include professional cleaning to remove tartar and plaque beneath the gums.
Home Dental Care Practices
Maintaining good oral hygiene daily is essential to prevent the buildup of plaque, which can exacerbate gum disease and diabetes. High blood glucose levels can lead to increased glucose in saliva, feeding harmful bacteria and escalating the risk of oral health problems.
- Brushing: Brush teeth twice a day with fluoride toothpaste.
- Flossing: Floss daily to remove plaque between teeth.
- Diet: Aim for a balanced diet to reduce the risk of cavities and to assist in diabetes management.
- Blood Glucose: Keep blood glucose levels within the target range to minimise the glucose level in the mouth fluids.
- No Smoking: Quitting smoking is strongly advised as it improves both oral and overall health.
- Hydration: Drink water regularly to alleviate symptoms of dry mouth.
If you have diabetes, book a check-up and clean to help prevent the onset of gum disease.